Jurisdiction Incident Management (Tier 3)

Jurisdiction incident management (Tier 3) is the primary site of integration of healthcare organizations (HCOs) with fire/EMS, law enforcement, emergency management, public health, public works, and other traditional response agencies. It provides the structure and support necessary for medical assets to maximize MSCC, and it allows direct input by medical representatives into jurisdictional action planning and decision-making. In addition, it links local medical assets with State and Federal support.
Key Points of the Chapter
Jurisdiction incident management (Tier 3) addresses MSCC at the level of the responding community. Earlier chapters focused on the management of individual healthcare assets (Tier 1) and on promoting cooperation among point-of-service medical providers (Tier 2). Tier 3 builds on this by describing the integration of public health and medical assets into the functional organization of incident command within the traditional emergency response community.
When a mass casualty and/or mass effect event occurs, multiple disciplines may be called into action, including public safety, public health, human services, emergency management, and others. Many of these disciplines do not routinely work together in this capacity and so are often unfamiliar with each other's emergency preparedness and response procedures. It is crucial, therefore, to establish incident management processes for jurisdictional (Tier 3) response that integrate the many diverse disciplines and promote coordinated response actions. This is accomplished through a well-organized and tested jurisdiction Emergency Operations Plan (EOP).
The basis for effective jurisdictional incident management (Tier 3) is the jurisdiction's Emergency Management Program (EMP). Public health and acute-care medical assets should be viewed as key components of the jurisdiction's EMP and should have direct input into preparedness and response planning. In times of crisis, jurisdictional management (Tier 3) will benefit from receiving a health and medical perspective on issues that determine incident objectives and response strategies. Moreover, individual HCOs may maximize their ability to provide MSCC through enhanced coordination with EMS and other community resources.
The integration of diverse organizations during incident response is best accomplished through unified incident command, a concept that allows multiple agencies to maintain significant management responsibility and to work together to achieve optimal response. A unified command approach promotes consistency throughout the response system. The participation of public health and medical disciplines in unified command at Tier 3 is important since they bear a primary responsibility for the welfare of responders and the general public.
4.1 The Role of the Jurisdiction in MSCC
Jurisdiction incident management (Tier 3) and its emergency management operations support are critically important to maximizing MSCC. In a mass casualty and/or mass effect event, Tier 3 is the management level that effectively coordinates activities among the multiple and disparate entities involved in response for that jurisdiction. Because of its obligation to the community, Tier 3 is responsible for defining incident objectives and an overall response strategy for the community. Data from various response disciplines are aggregated and analyzed at Tier 3. Thus, the jurisdictional information processing function is critical in promoting timely application of community resources to support urgent medical care at individual HCOs (Tier 1).
4.2 Jurisdiction Emergency Management Program
The jurisdictional EMP brings together the many agencies that have defined roles in emergency or disaster response, including public health and acute-care medical organizations (see below). It involves their active participation as a group in activities to mitigate, prepare for, respond to, and recover from mass casualty and/or mass effect events. It does not (and should not) preclude agencies from conducting their own EMP; rather, it provides a platform for individual efforts to be coordinated.
Participant Agencies/Organizations in the Jurisdiction Response:
- Emergency management
- Emergency Medical Services (EMS)
- Fire service (often combined with EMS)
- Local law enforcement (police, sheriff, and others)
- Public health and human services (often combined)
- Public works
- Acute medical services (hospitals, community health centers, nursing homes, outpatient clinics, private medical physician offices and other acute-care providers)
- Others, as determined by incident circumstances (e.g., school system, local Federal resources, such as Federal law enforcement, military assets, or Veterans Affairs facilities)
The jurisdictional EMP is best developed (and refined) through regular meetings of the leadership of each participant agency. These meetings should be conducted using formats similar to those developed for incident planning (i.e., there should be a designated leader/moderator, an agenda specifying the meeting objectives, defined processes for decision-making, and documentation of pertinent information and action items). The meetings allow participants to interact with one another and work toward common goals, just as they would be called on to do in an actual incident response.
An effective Tier 3 preparedness planning process accomplishes the following:
- Provides an opportunity for a jurisdiction's emergency response "players" to get to know one another and to understand each other's operations and perspectives
- Enables response disciplines to better understand the emergency procedures and methods that characterize each other's response domain
- Promotes a sense of trust between response disciplines
- Provides a forum for discussing issues or concerns and implementing effective methods to resolve differences fairly.
Similar to Tiers 1 and 2, a valid hazard vulnerability analysis (HVA) forms the cornerstone of the jurisdictional EMP. Findings of each response agency's HVA may be summarized to develop the jurisdiction's HVA, or a separate joint analysis may be performed. An integrated HVA provides an opportunity for agencies to assist one another in addressing collective and individual risk. It also gives advance warning of areas where certain agencies are particularly vulnerable. The jurisdiction's emergency management authority usually develops the jurisdiction's HVA, which should be reviewed and updated annually to address new or emerging threats to a population (e.g., construction of a chemical manufacturing plant).
Important insight is gained by incorporating public health and acute-care medical disciplines in the jurisdiction's HVA. In many jurisdictions, public health authorities have already undertaken HVA activities in accordance with State and Federally funded mandates related to bioterrorism. These efforts may help with examinations of risks that may complicate jurisdictional (Tier 3) response to a bioterrorism event. There will be common hazards identified and, potentially, common vulnerabilities. Most significantly, the medical sector may have vulnerabilities not recognized and addressed in the jurisdiction's regular planning process. This is important since jurisdictional planning usually assumes that HCOs will survive the hazard impact and be available to care for incident victims.
4.3 Jurisdiction Emergency Operations Plan
The jurisdictional EOP provides action guidance for incident response at the level of the responding community. The sum of all activities related to developing and implementing the jurisdictional EOP represents preparedness. This includes establishing equipment and supply needs, educating and training personnel, and exercising the system to evaluate and improve procedures. Important considerations for the jurisdictional EOP include:
- Developing all-hazards processes that can address potential incidents ranging from traditional weather events to large explosions, infectious disease outbreaks, or contamination scenarios
- Identifying essential participants in the jurisdictional EOP when it is implemented for a response
- Providing a systems description of how the various disciplines will be organized and integrated during response (may vary depending on the type of event), to include:
- Management structure and procedures for a multi-agency response
- Processes for information management and exchange among participants.
- Describing key responsibilities for each stage of response.
By incorporating basic ICS and emergency management principles, and by integrating public health and acute-care medical disciplines, a functional Tier 3 management structure is proposed.
Figure 4-1. Generic Management Structure for Jurisdictional Response
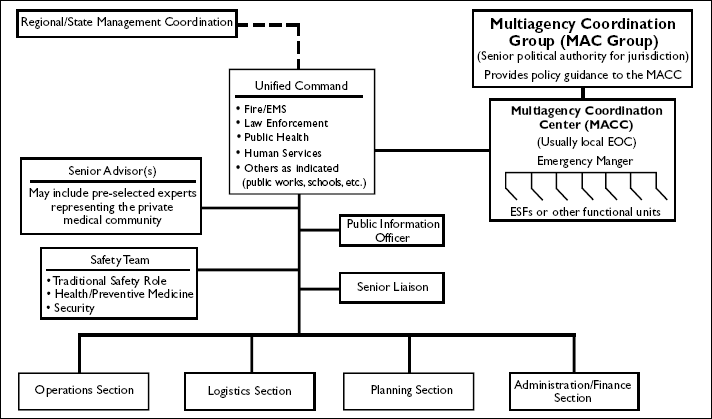
The site of integration for the Tier 2 liaison will vary based on the type of incident. In a mass casualty or complex medical event, the Tier 2 liaison will likely integrate at the Operations Section of the incident management team. In a primarily non-medical event, the Tier 2 liaison may integrate through the health and medical Emergency Support Function (ESF) or other functional group in the EOC (see
IS-701, Lesson 2).
4.4 Organization of the Tier 3 Response
The jurisdictional (Tier 3) response to a major medical incident is guided by the same general ICS principles as the Tier 1 response (i.e., it is organized by functional areas—Command, Operations, Logistics, etc.). However, responsibility for the five primary functions may be distributed among multiple agencies at the Tier 3 level. In many cases, collaborative efforts between disciplines are necessary to ensure that these functions are adequately addressed (see example below). This is particularly true for the Command function. Distinguishing features of the jurisdictional (Tier 3) response, are unified command and Multiagency Coordination Systems (MACS). These form the basis for the remainder of the chapter.
Example of Multiagency Unified Command During Incident Operations:
After recognition that a biological agent has been intentionally released into the community, public health may be designated as the lead agency in incident management, with primary responsibility for protecting the health and safety of the community. Public safety agencies also play a critical role by providing assistance to public health through their familiarity and expertise in ICS. They also support public health and medical operations. For example, the Logistics Section may consist primarily of fire service and public works resources providing support to public health by assisting epidemiological investigations or delivering prophylaxis medications to distribution centers.
Because multiple disciplines may have significant management roles in incident response, implementing a unified command (UC) is an effective way to promote cohesion within the response system. The UC facilitates information sharing and allows each involved discipline to provide input directly into the development of incident objectives and priorities. Although each agency's resources are integrated into the jurisdictional (Tier 3) operation, each agency retains individual authority over its assets and responsibilities. The disciplines most important to incorporate into the UC are those that primarily manage response in the jurisdictional EOP, including fire/EMS, law enforcement, public health, public works, and human services.
4.4.1.1 How Unified Command Works
Although the UC approach provides a certain level of equality among participants, a lead agency must be designated as the final arbiter in decision-making. This lead agency authority (a "first among equals") is determined by the type of incident according to guidelines established during preparedness planning (see example below). The lead agency should be clearly established at the outset of the incident response and publicized throughout the system so there is no doubt where the final decision authority rests.
Example of Lead Agency Designation Guidelines:
- Crisis/pre-hazard impact = Police department
- Hostage/standoffs = Police department
- Fires/explosions = Fire service
- Flash floods = Fire service
- HAZMAT release = Fire service
- Infectious disease = Public health
- Food contamination with illness = Public health
- Water contamination, utility disruption = Public works
Because strategic concerns may change as an incident evolves, the lead authority may be temporarily deferred, via open dialogue between UC participants, to another agency. In some cases, incident parameters may change enough to require a transfer of lead authority to another discipline. In a well-run UC, the decision to transfer lead authority is made during a management meeting using processes established for incident planning; it is documented and disseminated to all responders. Processes for deferring or transferring lead authority should be outlined during preparedness planning.
The site where the UC operates, the Incident Command Post (ICP), must be rapidly established and communicated to all agencies at the outset of a response. In any large-scale or multi-scene event, several ICPs may be estab-lished during the early reactive phase of response, with multiple disciplines involved. Identifying where the primary incident command is occurring—and how it integrates with the other command, operations, support, and information centers—should be prioritized as a critical incident-planning task.
Responsibility for specific functions under UC should also be defined using guidelines established during preparedness planning. The conduct of Safety, Liaison, and Public Information functions may be considered as follows:
- Safety Officer oversees all actions taken to protect responders, including issues related to the health (e.g., vaccination/prophylaxis) and security safety of responders. It may be best managed with input from a multidisciplinary group (i.e., Safety team) composed of the jurisdiction's (Tier 3) public health, EMS, law enforcement, and/or medical assets. The Safety team provides high-level input directly to incident management and has the authority to interrupt activities that appear unduly hazardous to responders.
- Senior Liaisons are assigned to agencies outside the jurisdictional ICS, such as jurisdictions adjacent to an affected community, or Federal agencies operating independently in an area. UC designates liaisons based on the type of incident and the agencies involved. For example, during response to a terrorist act involving an infectious disease outbreak, a senior public health official might be assigned as a liaison to the Joint Field Office (JFO). Assignments may vary from one incident to the next, and as incident parameters change, but liaison staff should remain consistent during an incident to promote continuity of interactions.
- Public Information Officer (PIO) serves as the official spokesperson for the jurisdiction (Tier 3) response, talking specifically about the incident and providing official incident-related data. Moreover, the PIO monitors the media message and the public's reaction in an effort to detect rumors and correct misinformation. The PIO should not usurp the responsibility of the PIO from the jurisdiction's political authority or from the Emergency Operations Center (EOC). Thus, processes should be established during preparedness planning to ensure coordination among these entities in developing the media message. As with safety, multidisciplinary input to this task is generally preferred, with the lead PIO assigned according to the lead authority in the UC.
4.4.1.2 Medical Participation in Unified Command
During a large-scale event, especially one with a primarily medical focus, acute-care medicine should be involved in incident command decisions and defining the response objectives. UC, therefore, must allow for direct input from a jurisdiction's medical community.[51] This can be accomplished either by including medicine as a formal participant in the UC (with fire/EMS, human services, law enforcement, etc.), or by establishing a senior advisory role for medicine to the UC. Because most medical assets are privately owned (and therefore lack legal protection for public action during incident response), the senior advisory approach may be preferred.
Figure 4-1 (presented in section 4.3) illustrates the senior advisory concept and how it fits into the UC. The medical representatives who serve as advisors may come from the healthcare coalition (Tier 2) or be jointly selected by the jurisdiction's medical community. The role of these "trusted agents" must be clearly defined during preparedness planning. They should be chosen based, in part, on their ability to represent the collective interests and concerns of all health and medical organizations in the jurisdiction when presenting recommendations to incident command. In addition, the medical advisors should have operational medicine experience and be well versed in the principles of ICS.
The advisory group should be notified and available on request to provide advice throughout an incident; however, its input is most critical when incident circumstances require the medical community to significantly alter its normal operations (e.g., asking HCOs to adhere to unusual isolation procedures in a prolonged disease outbreak). Although medical advisors report incident information back to their constituents, they are not responsible for providing jurisdictional (Tier 3) management with updates on the status of HCOs. This should occur through a defined process within the Planning Section of the jurisdictional ICS.
Operations, Logistics, Planning, and Administration/Finance Sections will likely also require multiple disciplines to collaborate using a unified methodology. The managers of these sections, typically known as "Chiefs," make up the "general staff" of the jurisdictional (Tier 3) response. The Incident Commander (or lead authority in the UC team) appoints Section Chiefs at the outset of response from a pool of candidates identified and trained during preparedness planning. The Chiefs are usually senior members of the lead authority agency/organization who have significant experience in emergency or disaster response and demonstrated management expertise in ICS.
Specific activities of the four sections are as follows:
- Operations Section develops the tactics and assignments to accomplish operational period objectives set by the incident commander. In a jurisdictional (Tier 3) response, several "branches" within Operations may be necessary to organize assets responsible for public health and medical issues. For example, Operations branches that may be indicated during a major medical incident, are highlighted in Figure 4-2 below along with brief descriptions of the activities for which each branch is responsible.[52] The activation of Operations branches will depend on incident circumstances and, in fact, most incidents will not require all branches.
- Logistics Section manages activities that provide support through equipment and supplies, transportation, personnel, processing of volunteers, and technical activities to maintain the function of operational facilities. For example, Logistics would help in receiving, transporting, and protecting a cache from the Strategic National Stockpile (whereas Operations focuses on providing prophylactic medications to the at-risk population).
- Planning Section supports Command and Operations in processing incident information and developing incident action plans (IAPs) for the response. It is responsible for collecting, analyzing, and disseminating aggregate data, and maintaining up-to-date documentation of resource status. The Planning Section must specifically address:
- Support for incident command in carrying out planning meetings (e.g., set meeting schedule, develop an agenda, ensure that objectives are established, incorporate decisions into the IAP)
- Event projections (based on the known characteristics of the hazard and its historical impact, if there is one)
- Evaluation of response progress by monitoring valid measures of effectiveness.[53]
- Contingency and long-range planning
- Demobilization planning
- Support to complete each IAP (e.g., writing, printing).
- In addition, the Planning Section manages multiple types of information in a major health or medical response including:
- Situation status: Incident parameters (e.g., numbers of victims, locations, types of injury or illness)
- Resource status: Response asset parameters (e.g., tracking such resources as staffed beds available at local hospitals, quantities of a particular prophylaxis for distribution)
- Recommendations and directives (e.g., informing responders and the general public about evaluation and treatment protocols).
- Administration/Finance Section supports Command and Operations in administrative issues and in tracking and processing incident-related expenses. Examples of the issues that might be of concern for the public health and medical disciplines include:
- Practitioner licensure requirements
- Regulatory compliance issues, including the possible temporary suspension of certain regulations during the period of emergency (as indicated)
- Financial accounting during an incident
- Contracting for services and supplies directly available to incident managers.
Figure 4-2. Operations Branches for Medical and Public Health Assets
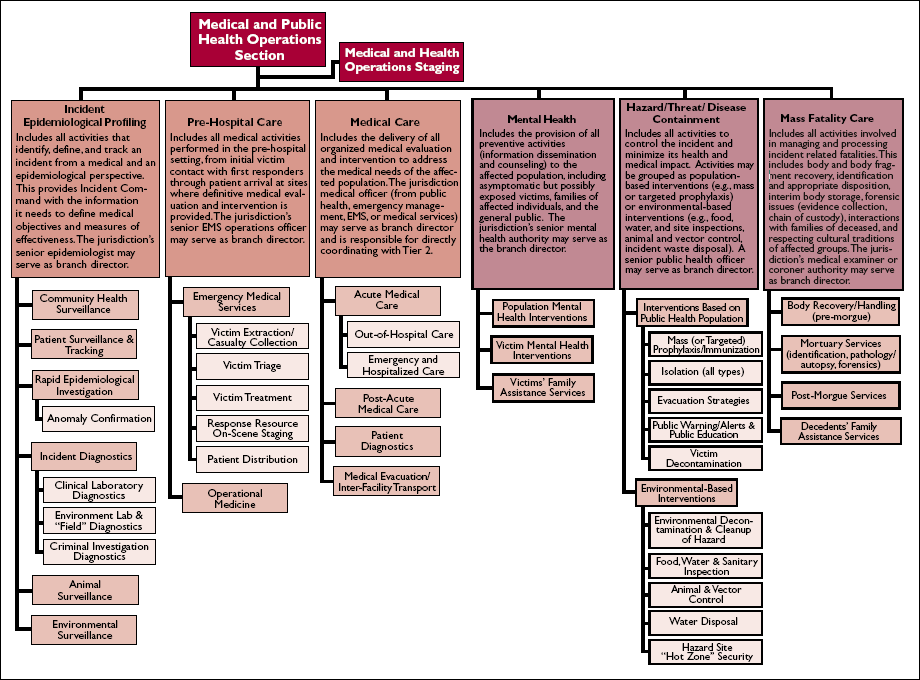
More information on individual Operations branches.
Adapted from J.A. Barbera and A.G. Macintyre. Medical and Health Incident Management (MaHIM) System: A Comprehensive Functional System Description for Mass Casualty Medical and Health Incident Management. Institute for Crisis, Disaster, and Risk Management, the George Washington University. Washington, DC, October 2002.
More information on individual Operations branches.
4.5 Integration of Incident Management and Emergency Management
Emergency management operations support to the UC occurs through the jurisdiction's Multiagency Coordination Center or MACC, which is commonly based at an EOC. The EOC is the pre-designated facility in a jurisdiction from which emergency management personnel and government officials exercise direction and control in an emergency and provide high-level support to the UC. In the traditional disaster scenario, the UC operates from an ICP at the incident scene (e.g., site of a building collapse), and is geographically separated from the EOC.
Figure 4-3. EOC Incident Support in Traditional Emergency Response
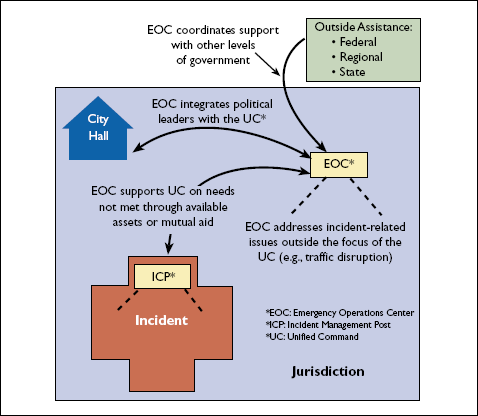
If the incident is diffuse, involves the entire jurisdiction, or in some other way prevents the UC from establishing its ICP elsewhere, the EOC may provide the structure and function for the ICP. When this occurs, the UC should occupy a space that is separate from emergency management operations support personnel so the focus of the UC remains distinct from that of the local emergency management and the MACS. However, the EOC leadership (in many cases, this is the local emergency manager) should attend and participate in the UC planning meetings and operations briefings, and related activities.[54] This integrates the UC with the local jurisdiction's MACS, but avoids risking crossover/conflict between their designated response roles. It also empowers the EOC to more actively support the UC by better anticipating possible incident response needs.
4.6 Integration With Other Tiers
The jurisdictional (Tier 3) response system integrates with other tiers primarily through its information management function. The capability to collect, analyze, and disseminate aggregated data should always be operational, even if only at a baseline level during times of non-response. This enables healthcare coalition (Tier 2) leaders to be notified of upcoming meetings or changes to the jurisdictional response system. It also facilitates timely incident response by providing key medical personnel (e.g., Tier 2 coalition managers) with the earliest reports of hazards that may have significant medical implications.
During incident response, a robust jurisdictional (Tier 3) information management function within the Planning Section continually processes data received from the Tier 2 coalition to obtain real-time situation status on HCO operations. This situation status information is reported back to the data sources and is also used for Tier 3 incident action planning. Integration of this information into jurisdictional (Tier 3) action planning, and providing jurisdiction IAP action plan information to the HCOs promotes coordination of response actions between tiers. For example, plans to shut down roads or public transportation systems in an area may greatly affect the ability of healthcare personnel to reach local HCOs. Having this concern communicated via the Tier 2 liaison to the UC is beneficial in helping Operations Section personnel under UC (or in the EOC) develop tactics that will not interfere with HCO activities. In a similar way, an adequate information management function can provide much needed guidance to medical practitioners during an incident.
Example: In an unusual infectious disease outbreak, a jurisdiction's public health authority may issue health advisories that contain practitioner guidelines on patient evaluation, treatment modalities, and methods for reporting suspect cases. Medical practitioners benefit from the ability to access this information as incident circumstances evolve because it is both medically sound and it carries jurisdictional public health authority for implementation. The application of this guidance across a jurisdiction promotes hazard impact containment through evaluation and treatment efficiency and consistency, data reporting for incident profiling, and indications for altering or improving medical therapy or other recommendations.
The
New York City Department of Health and Mental Hygiene website is an excellent public health model for disseminating accurate, timely, and authoritative medical guidance.
The jurisdictional (Tier 3) ICS integrates with State authorities (Tier 4) primarily through its information management function. Timely processing and dissemination of incident and response parameters enable the Governor to determine the need for declaring a formal emergency or requesting Federal support. Such information also makes it possible to link affected intrastate jurisdictions so they can coordinate response efforts. Finally, it facilitates the coordination and distribution of State tactical mutual aid to areas with the greatest need.
The integration of jurisdictional and State entities with responsibility for emergency preparedness and response is a primary mission of several Federal initiatives. One example is the DHS-funded Metropolitan Medical Response System (MMRS) program. The MMRS provides funding and guidance to select highly populated jurisdictions (124 as of FY 2003) to develop plans, conduct training and exercises, and acquire pharmaceutical caches, PPE, and other capabilities necessary to respond to a mass casualty and/or mass effect event. It also requires planning integration with State (Tier 4), neighboring interstate jurisdictions (Tier 5), and Federal (Tier 6) entities. The MSCC Management System provides an effective platform for health and medical disciplines to coordinate/integrate capabilities acquired or developed through the MMRS.
4.7 Illustrative Example
The following example demonstrates how the concepts presented in this chapter may be applied during an actual incident response. The various phases of response (as described in
Chapter 1) highlight when critical actions should occur; however, the example extends only as far as incident response operations, as this is the focus of the MSCC Management System.
Background and Incident Description
- Jurisdiction Alpha is a city of moderate size whose western border adjoins another State.
- A very sick patient with severe respiratory distress and a fever is admitted to a hospital in Jurisdiction Alpha. His admission was preceded by nearly three days of progressive illness with cough. During this time, he continued to work as a butcher in a small but popular meat shop. Since the patient had recently returned from an overseas trip to areas where severe acute respiratory syndrome (SARS) had reappeared, SARS is suspected and the jurisdiction's Department of Health (DoH) is notified.
- The patient dies a short time after his admission to the hospital.
Incident recognition begins when the clinical suspicion is first reported to DoH and public health experts recognize the implications. Although it has not been confirmed, the suspicion of SARS is enough to warrant immediate actions by DoH, and a rapid health investigation commences. Epidemiological questioning quickly indicates that the patient (index case) had exposure to many customers at the meat shop after becoming demonstrably ill.
Notification/activation occurs when the DoH public health officer requests a management meeting with representatives from emergency management, fire/EMS, law enforcement, and public works. After a brief discussion, they agree to partially activate Jurisdiction Alpha's EOP for public health response (formal declaration of emergency is not required to activate portions of the EOP). The following actions also occur:
- Using the jurisdiction's public safety communications center (as specified in the EOP), a written communication is sent to all agencies that automatically participate in the EOP. The notification only activates jurisdictional resources that are needed for the initial response.
- An alert is issued to all HCOs in the jurisdiction (through Tier 2) indicating what is known about the demographics and recent history of the index patient, and any reported outbreaks elsewhere in the United States. The alert notifies Tier 2 assets that the jurisdiction EOP is partially activated.
- A similar notification is provided to the State DoH, which notifies neighboring regions and the CDC using mechanisms established in Tiers 4, 5, and 6.
- The mayor and city council are notified and immediately express concern. They recognize the potential human impact, as well as the implications for business and tourism. The mayor's PIO works with the DoH PIO to draft and immediately release a statement to the public explaining the jurisdiction's response.
Mobilization of jurisdictional resources occurs as the designated agencies activate their individual EOPs, and ramp up their staffing accordingly. Similarly, Jurisdiction Alpha's EOC is activated and staffed.
Incident operations are led by a UC that was designated in the initial management meeting. The UC is composed of selected individuals from jurisdictional (Tier 3) public health, fire/EMS, and law enforcement. The jurisdiction's public health authority is recognized as the "lead" UC agency. The UC coordinates closely with the jurisdiction's emergency manager, who manages the EOC (a MACC for the UC).
Management representatives from each agency in the UC conduct a teleconference to discuss what is known about the incident and to determine a course of action. It is decided that an ICP will be established at the DoH Operations Center, but UC members agree to transfer the ICP to the jurisdiction's EOC if management needs exceed the resources available at the DoH Operations Center. This backup is planned because multiple reports are coming in about patients with febrile illnesses reporting to HCOs. Many of these patients have recently visited the butcher shop in question.
Members of the UC quickly establish themselves at the ICP and coordinate the integration of their respective disciplines. Each agency maintains authority over its own assets, yet all contribute to the composition of the ICS Sections (Operations, Logistics, Plannings, Admin/Finance). For example, a senior DoH staff member directs the Operations Section, while personnel from other agencies manage specific branches (see Figure 4-2) under Operations.
- A jurisdictional epidemiologist manages the Incident Epidemiological Profiling and Hazard Containment branches, with additional resources supplied by other agencies.
- EMS manages Pre-Hospital Care.
- A trained, experienced medical administrator pre-selected by thethe Tier 2 coalition serves as a senior medical advisor to the UC for issues related to hospital care. This role is designed to provide the hospital and medical practitioners' "perspective" when the UC is considering jurisdictional decisions that will affect the provision of incident-related medical care.
- A jurisdictional medical examiner manages Fatality Care.
Expedited SARS serology tests from the index patient strongly indicate the patient died from SARS. Confirmatory testing is being conducted at the CDC. The rapid epidemiological investigation, aided by public service announcements asking anyone in contact with the meat shop to report to a DoH clinic for evaluation, has identified an extensive list of potential contacts. The contacts are given written instructions on the disease, its signs and symptoms, and precautionary measures. They are provided digital thermometers and arrangements are made to contact them daily for a health check.
Based on available information, the UC develops the first formal jurisdictional IAP for the next opertional period (designated as the upcoming 24-hour period starting at 7:00 a.m.). The jurisdictional IAP includes:
- Control objectives for the overall response
- Operational period objectives
- Strategies for achieving the objectives, including:
- Disease containment for healthcare workers, identified contacts of the index case, and the general public
- Surveillance of the health of identified index case contacts
- Surveillance of HCOs and medical providers to identify other cases of possible SARS in the jurisdiction
- Contingency planning for medical surge needs (e.g., hospital isolation, critical care services, screening of concerned members of the public)
- Concise public information bulletins that are consistent across all tiers.
- Response tactics, including:
- Twice daily telephonic screening of identified contacts, looking for early symptoms
- Educational information for identified case contacts
- Voluntary separation of contacts, with health personnel to assist and ensure that they maintain their separation from the public
- Educational information and personal protection supplies for family members who remain at home during the contact's period of voluntary separation
- Educational information for healthcare providers describing the early signs, symptoms, and physical findings of SARS. Contact information is also provided to report suspected cases, including how to obtain expedited serologic testing.
- Educational information for the public.
- Situation status and resource status updates for the jurisdiction
- Chart illustrating the jurisdiction's incident command organization, with the primary role of each agency and other significant participants specified; contact information is provided; the chart also demonstrates the relationship of UC to the EOC and to department operations centers.
- Communications and safety plans, including DoH recommended protection (e.g., PPE, isolation, other protective measures for persons caring for potential SARS victims).
The jurisdictional IAP is shared with Tier 2 coalition members and State emergency management officials (Tier 4). The State, in turn, provides pertinent information to adjoining jurisdictions, bordering States, and to Federal public health personnel assisting in the State response. The operational period established by the State is adjusted so that State meetings occur one hour after the jurisdiction's (Tier 3) meetings. This phase-shift of Tier 4's operational period allows for coordination of operational briefings.
With the UC having defined its incident objectives and strategies through the jurisdictional IAP, other activities are identified for emergency management operations support to address through the EOC. These EOC responsibilities include:
- Interfacing with the private sector (excluding hospitals, which are considered part of incident operations)
- Interfacing with the State and the Federal Government (except for Federal health and medical resources that consult to, or work under, the jurisdiction's management system)
- Determining school closures, addressing transportation disruptions, and managing other SARS impacts on the jurisdiction
- Providing interface of UC with MAC Group (mayor and her senior advisors).
51. Hospitals, integrated healthcare systems, clinics, alternative care facilities, nursing homes and other skilled nursing facilities, private practitioners' offices, and other assets constituting Tier 1 in the MSCC Management System represent the medical community.
52. This example is adapted from the
Medical and Health incident Management (MaHIM) System.
53. Measures of effectiveness are observable criteria that management accepts as accurate and valid reflections that incident response is accomplishing its objectives. They should be defined in the planning process and used in the situation status reports.
54. When the UC is operating at a distant incident scene, EOC leadership could still participate in UC planning meetings via teleconference or some other defined mechanism. This is helpful in promoting full coordination between incident command and emergency management operations support.

