Key Points of the Chapter
Mass casualty and/or mass effect[12] incidents create demands that often challenge or exceed the medical infrastructure of an affected community. A mass effect incident may be defined as a hazard impact that primarily affects the ability of the organization to continue its usual operations (in contrast to a mass casualty incident). For healthcare systems, the usual medical care capability and capacity can be compromised and the ability to surge prevented. The ability to provide adequate medical care under such circumstances is known as medical surge. There are two components of medical surge: (1) surge capacity is the ability to respond to a markedly increased number of patients; (2) surge capability is the ability to address unusual or very specialized medical needs. Strategies to enhance medical surge capacity and capability (MSCC) require a systems-based approach that is rooted in interdisciplinary coordination and based at the local level.
The MSCC Management System describes a framework of coordination across six tiers of response, building from the individual healthcare organization (HCO) and its integration into a local healthcare coalition, to the integration of Federal public health and medical support. The most critical tier is jurisdiction incident management (Tier 3) since it is the primary site of integration for public health and medical assets with other response disciplines. Each tier must be effectively managed internally in order to integrate externally with other tiers.
Emergency management and Incident Command System (ICS) concepts form the basis of the MSCC Management System. Within ICS, response assets are organized into five functional areas: Command establishes the incident goals and objectives (and in so doing defines the incident); Operations Section develops the specific tactics and executes activities to accomplish the goals and objectives; and the Planning, Logistics, and Administration/Finance Sections support Command and Operations. The Planning Section is particularly critical because it manages complex information across tiers and facilitates information exchange among responders to promote consistency within the overall system.
Because multiple agencies may have leadership responsibilities in a mass casualty and/or mass effect incident, a unified command approach is essential. Unified command enables disparate entities (both public and private) to collaborate and actively participate in the development of incident goals, objectives, and an overarching response strategy. Participation by public health and medical disciplines in unified command is important since these disciplines have a primary responsibility for ensuring the welfare of responders and the general public. Where unified command is not implemented due to sovereignty issues (e.g., across State borders or between private facilities), effective mechanisms for management coordination should be established.
1.1 What is Medical Surge
The concept of medical surge forms the cornerstone of preparedness planning efforts for major medical incidents. It is important, therefore, to define this term before analyzing solutions for the overall needs of mass casualty or mass effect incidents.
Medical surge describes the ability to provide adequate[13] medical evaluation and care during events that exceed the limits of the normal medical infrastructure of an affected community. It encompasses the ability of HCOs to survive a hazard impact and maintain or rapidly recover operations that were compromised (a concept known as medical system resiliency).
Beyond this rather simple explanation, medical surge is an extraordinarily complex topic that is difficult to comprehensively describe. The first step in doing so, however, is to distinguish surge capacity from surge capability.
Medical surge capacity refers to the ability to evaluate and care for a markedly increased volume of patients—one that challenges or exceeds normal operating capacity. The surge requirements may extend beyond direct patient care to include such tasks as extensive laboratory studies or epidemiological investigations.
Because of its relation to patient volume, most current initiatives to address surge capacity focus on identifying adequate numbers of hospital beds, personnel, pharmaceuticals, supplies, and equipment. The problem with this approach is that the necessary standby quantity of each critical asset depends on the systems and processes that:
- Identify the medical need
- Identify the resources to address the need in a timely manner
- Move the resources expeditiously to locations of patient need (as applicable)
- Manage and support the resources to their absolute maximum capacity.
In other words, fewer standby resources are necessary if systems are in place to maximize the abilities of existing operational resources. Moreover, the integration of additional resources (whether standby, mutual aid, State or Federal aid) is difficult without adequate management systems. Thus, medical surge capacity is primarily about the systems and processes that influence specific asset quantity.
Basic example: If a hospital wishes to have the capacity to medically manage 10 additional patients on respirators, it could buy, store, and maintain 10 respirators. This would provide an important component of that capacity (other critical care equipment and staff would also be needed), but it would also be very expensive for the facility. If the hospital establishes a mutual aid and/or cooperative agreement with regional hospitals, it might be able to rely on neighboring hospitals to loan respirators and credentialed staff and, therefore, might need to invest in only a few standby items (e.g., extra critical care beds), minimizing purchase and maintenance of expensive equipment that generate no income except during rare emergency situations.
When addressing an overall medical surge strategy, it is recommended that guidance be delineated prospectively for maximizing the use of existing resources before resorting to the use of alternate care facilities and standards of care appropriate to the austere conditions of a disaster.[14]
Medical surge capability refers to the ability to manage patients requiring unusual or very specialized medical evaluation and care. Surge requirements span the range of specialized medical services (expertise, information, procedures, equipment, or personnel) that are not normally available at the location where they are needed (e.g., pediatric care provided at non-pediatric facilities). Surge capability also includes patient problems that require special intervention to protect medical providers, other patients, and the integrity of the HCO.
Basic example: Many hospitals encountered difficulties with the arrival of patients with symptoms of severe acute respiratory syndrome (SARS). The challenge was not presented by a high volume of patients, but rather by the specialty requirements of caring for a few patients with a highly contagious illness that demonstrated particular transmissibility in the healthcare setting. Protection of staff and other patients was a high priority, as was screening incoming patients and staff for illness, preventing undue concerns among staff, and avoiding publicity that could adversely affect the hospital's business. Coordination with public health, emergency management, and other response assets was critical.
Effective strategies for MSCC require a systematic approach to meet patient needs that challenge or exceed normal operational abilities, while preserving quality of care and the integrity of the healthcare system. The MSCC Management System demonstrates management processes that allow HCOs to coordinate existing resources and then obtain "outside" assistance in a timely and efficient manner. In this way, HCOs can transition from baseline operations to incident surge capacity and capability—to meet the response needs of catastrophic events—and then back to baseline.
Figure 1-1. Management System for Reaching MSCC Objectives

Any strategy to enhance MSCC must recognize that the required emergency interventions are time sensitive and must be based primarily at the local level. This urgency limits the ability of the Federal Government to independently establish, stockpile, or own/control resources necessary for immediate MSCC. In addition, because most medical assets in the United States are privately owned, MSCC strategies must bridge the public-private divide, as well as integrate multiple disciplines and levels of government.
A comprehensive effort to address response requirements must include a system description (i.e., how the different response components are organized and managed) and a concept of operations (i.e., how the system components function and interact through successive stages of an event). It must include "all-hazard" processes and procedures, mutual aid, and other validated emergency management concepts. The remainder of this chapter presents key considerations for the system design and the concept of operations to maximize integration between response components and, thus, enhance MSCC.
1.2 The MSCC Management System
The MSCC Management System describes a system of interdisciplinary coordination that emphasizes responsibility rather than authority. In other words, each public health and medical asset is responsible for managing its own operations, as well as integrating with other response entities in a tiered framework. This allows response assets to coordinate in a defined manner that is more effective than the individual, ad hoc relationships that otherwise occur during a major emergency or disaster.
The six-tier construct (Figure 1-2) depicts the various levels of public health and medical asset management during response to mass casualty and/or mass effect incidents. The tiers range from the individual HCO or other healthcare assets and their integration into a local healthcare coalition, to the coordination of Federal assistance. Each tier must be effectively managed internally in order to coordinate and integrate externally with other tiers.
Figure 1-2. MSCC Management Organization Strategy
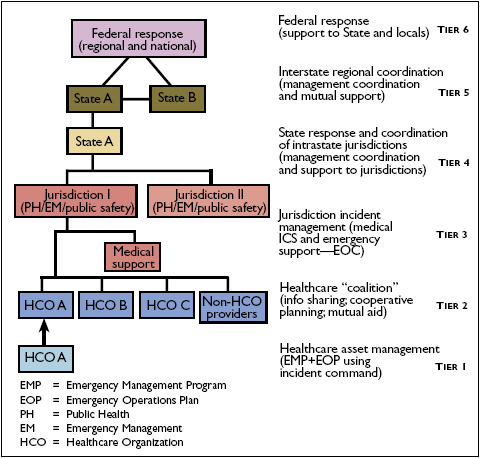
Tier 1 includes hospitals, integrated healthcare systems, private physician offices, outpatient clinics, nursing homes and other skilled nursing facilities, and other resources where "point of service" medical care is provided. Emergency Medical Services (EMS) may be included in Tier 1 if called on to provide field-based medical care in an emergency. The goal of Tier 1 is to maximize MSCC within each healthcare asset while ensuring the safety of personnel and other patients, and the integrity of the asset's usual operations. This is best accomplished by optimizing an entity's Emergency Operations Plan (EOP) to effectively manage internal resources and to integrate with external response assets. The MSCC Management System describes key considerations for internal preparedness planning, while focusing primarily on the processes within the EOP that facilitate external integration with the larger response community.
The healthcare coalition organizes individual healthcare assets into a single functional unit. Its goal is to maximize MSCC across the coalition through cooperative planning, information sharing, and management coordination. The coalition ensures that public health and medical assets have the information and data they need at a level of detail that will enable them to optimally provide MSCC. In addition to hospitals, the coalition may include long-term care or alternative treatment facilities, dialysis and other outpatient treatment centers, nursing homes and other skilled nursing facilities, private physician offices, clinics, community health centers and any other healthcare asset that may be brought to bear during major medical response. Its reach may extend beyond the geographic area of the primary responding jurisdiction (Tier 3), especially in rural settings where healthcare assets may be scattered.
Tier 2 strengthens MSCC by creating the ability to move medical resources (e.g., personnel, facilities, equipment, supplies) to sites of greatest need.[15] This is accomplished through mutual aid and cooperative agreements[16] between HCOs. It also provides a platform for unified interface with the jurisdiction's incident management (Tier 3). To be effective, the coalition must establish a planning process that is equal and fair to all participants, giving each the opportunity for input during preparedness planning, response, and recovery.
Tier 3 directly integrates HCOs with other response disciplines (e.g., public safety, emergency management) to maximize jurisdictional MSCC. It is the most critical tier for integrating the full range of disciplines that may be needed in a mass casualty and/or mass effect incident. The focus of Tier 3 is to describe how to effectively coordinate and manage diverse disciplines in support of medical system resiliency and medical surge demands. This requires healthcare assets to be recognized as integral members of the responder community and to participate in management, operations, and support activities. In other words, public health and medical disciplines must move from a traditional support role based on an Emergency Support Function (ESF) to part of a unified incident command system. This is especially important during events that are primarily public health and medical in nature, such as infectious disease outbreaks.
To address MSCC, Tier 4 describes how State-level actions can support jurisdiction incident management (Tier 3), promote coordination among multiple affected jurisdictions, or assume a primary incident command role. The State management function also serves as the primary interface for requesting Federal assistance. During preparedness planning, State agencies may facilitate arrangements between jurisdictions to coordinate response assets. The use of strategic mutual aid and/or cooperative agreements may standardize the implementation of tactical mutual aid between jurisdictions and promote a cohesive response strategy during a widespread incident.
Tier 5 describes how to maximize interstate coordination to support MSCC. In the past, interstate coordination generally depended on ad hoc arrangements, goodwill at the time of an incident, and other less-than-predictable mechanisms. However, this changed when Congress enacted the Emergency Management Assistance Compact in 1996 (Public Law 104-321). EMAC, as it is commonly known, has now been accepted by all States and U.S. territories, and provides legal authority, financial mechanisms, and operational guidance to establish the ability to request and receive emergency assistance from other States or territories. This tier focuses on how to manage interstate medical and public health assistance and examines how mutual aid, incident management coordination, and information sharing can enhance MSCC.
The Federal Government maintains public health and medical resources to support State, Tribal, and jurisdictional authorities during a mass casualty and/or mass effect incident. The goal of Tier 6 is to maximize MSCC through the optimal integration and management of Federal public health and medical assets. Activation of Federal public health and medical assistance may occur through implementation of the Robert T. Stafford Disaster Relief and Emergency Assistance Act (424 USC 5121, et seq.) or through independent authority of the Department of Health and Human Services (HHS) to declare a Federal public health emergency or disaster.[17] The National Response Plan (NRP) and National Incident Management System (NIMS) provide operational guidance for Federal action. Tier 6 focuses on key functional concepts that promote integration of the Federal response.
1.3 Emergency Management and the Incident Command System
Emergency management and Incident Command System (ICS) concepts serve as the basis for the MSCC Management System.[18] However, unlike traditional descriptions of emergency management and ICS, which organize assets around a defined scene, the MSCC Management System has adapted the concepts to be more applicable to large-scale medical and public health response where there is no defined scene, or where multiple incident scenes may exist (e.g., infectious disease outbreak). Public health and medical professionals must understand the utility of emergency management and ICS concepts as they relate to public health and medical disciplines.[19]
The following pages examine key distinctions between emergency management and ICS and the roles that each is designed to fulfill during a major medical incident.
Emergency management describes the science of managing complex systems and multidisciplinary personnel to address extreme events, across all hazards, and through the phases of mitigation, preparedness, response, and recovery. Hospital staff and other healthcare personnel might equate emergency management activities to a hospital's Disaster Committee (hence the recommended name change to Emergency Management Committee). The sum of all emergency management activities conducted by a response organization may be collectively referred to as an Emergency Management Program (EMP) for that entity. The term program is used because it denotes activity that is continuously ongoing, whereas a plan is often considered a series of actions that occur only in response to defined circumstances.
The activities of the EMP address the phases of mitigation, preparedness, response, and recovery. They are based on a hazard vulnerability analysis (HVA), which if properly accomplished, will identify potential hazards, assess their likelihood of occurrence, their potential impact and the organization's vulnerabilities to the impact, and provide a basis for understanding how the hazard likelihood and organizational vulnerabilities can be addressed. Each EMP phase is briefly described below.
- Mitigation encompasses all activities that reduce or eliminate the probability of a hazard occurrence, or eliminate or reduce the impact from the hazard if it should occur. In Comprehensive Emergency Management, mitigation activities are undertaken during the time period prior to an imminent or actual hazard impact. Once an imminent or actual hazard impact is recognized, subsequent actions are considered response actions and are not called "mitigation." This avoids the confusion that occurs with the HAZMAT discipline's use of mitigation, which applies to response actions that reduce the impact of a hazardous materials spill. Mitigation is the cornerstone of emergency management because any response strategy relies on medical assets surviving a hazard and maintaining operations in the post-impact environment (i.e., medical system resiliency). An effective mitigation effort should begin with, and be based on, a valid HVA as this will help an organization prioritize issues during follow-on mitigation and preparedness planning.
- Preparedness encompasses actions designed to build organizational resiliency and/or organizational capacity and capabilities for response to and recovery from hazard impacts. It includes activities that establish, exercise, refine, and maintain systems used for emergency response and recovery. The critical task in preparedness planning is to define the system (how assets are organized) and processes (actions and interactions that must occur) that will guide emergency response and recovery. This is accomplished through the development of an effective EOP (see below for suggested EOP formats). Staff should be educated and trained on the system so they gain the knowledge and skills necessary to adequately perform their assigned roles.
- It is important to note that the procedures and systems used to conduct preparedness activities (committee structure and meetings, memo writing, regular email notification of meetings, etc.) are typically not adequate for use during emergency response. This point is often missed by organizations as they attempt to utilize emergency preparedness committees and their associated structures and processes to manage response to an event. The EOP defines effective process and procedures for the context of emergency response (emergency notification procedures, establishing an incident management team, processing of incident information, etc.). It is recommended that, to the extent possible, emergency response process and procedures be used to conduct preparedness activities.[20]
- Response activities directly address the hazard impact, including actions taken in anticipation of an impending event (e.g., hurricane, tornado) and actions during and after an impact has occurred. Specific guidance for incident response, including processes for asset deployment, is addressed in an EOP. An effective EOP not only guides the initial (reactive) response actions but also promotes transition to subsequent (proactive) incident management.
- Recovery activities restore the community to "normal" after a major incident. The initial recovery stage (which actually begins in the late stages of response) is integrated with response mechanisms, and the EOP incident management process should be extended into recovery. The management transition from response to recovery (both timing and methods) must be carefully planned and implemented to avoid problems. As recovery progresses, recovery management transitions to regular agency management processes or some intermediate method defined by the responsible organizations.
The ICS provides guidance for how to organize assets to respond to an incident (system description) and processes to manage the response through its successive stages (concept of operations). All response assets are organized into five functional[21] areas: Command, Operations, Planning, Logistics, and Administration/Finance. Figure 1-3 highlights the five functional areas of ICS and their primary responsibilities.
Figure 1-3. Incident Command System
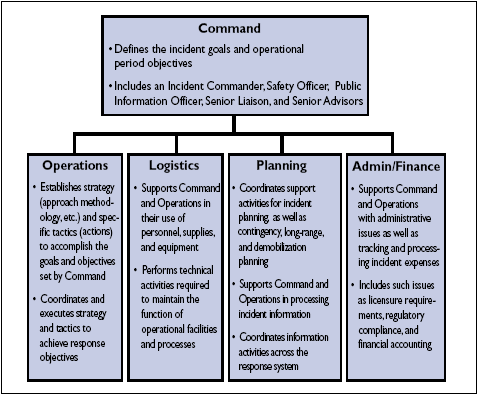
The ICS, as described in NIMS, refers to the combination of facilities, equipment, personnel, procedures, and communications operating within a common organizational structure and designed to aid in the management of resources during incident response. The ICS is based on eight concepts that contribute to the successful application of this system.
Exhibit 1-3. Incident Command System Core Concepts
-
Common terminology - use of similar terms and definitions for resource descriptions, organizational functions, and incident facilities across disciplines.
-
Integrated communications - ability to send and receive information within an organization, as well as externally to other disciplines.
-
Modular organization - response resources are organized according to their responsibilities. Assets within each functional unit may be expanded or contracted based on the requirements of the event.
-
Unified command structure - multiple disciplines work through their designated managers to establish common objectives and strategies to prevent conflict or duplication of effort.
-
Manageable span of control - response organization is structured so that each supervisory level oversees an appropriate number of assets (varies based on size and complexity of the event) so it can maintain effective supervision.
-
Consolidated action plans - a single, formal documentation of incident goals, objectives, and strategies defined by unified incident command.
-
Comprehensive resource management - systems in place to describe, maintain, identify, request, and track resources.
-
Pre-designated incident facilities - assignment of locations where expected critical incident-related functions will occur.
For ICS to be effective, the incident must be formally defined so that there is clarity and consistency as to what is being managed. This may be best accomplished by defining the incident response through delineation of response goals and objectives, and by explaining response parameters through an Incident Action Plan (IAP)—the primary documentation that is produced by the incident action planning process.[22]
Early in the response to the Pentagon on 9/11, incident command (headed by the Arlington County, VA, Fire Department) defined the incident as managing the fire suppression, building collapse, and the search and rescue activities at the Pentagon. It did not include objectives for managing the disruption of traffic or other countywide ramifications of the plane crash. Arlington County emergency management officials, therefore, quickly knew they had to manage these other problems through their Emergency Operations Center (EOC), which was geographically separate from, but closely coordinated with, incident command at the Pentagon.
The utility of ICS becomes evident when analyzing the demands encountered during an incident response.
Figure 1-4. Types of Demands Encountered in Incident Response
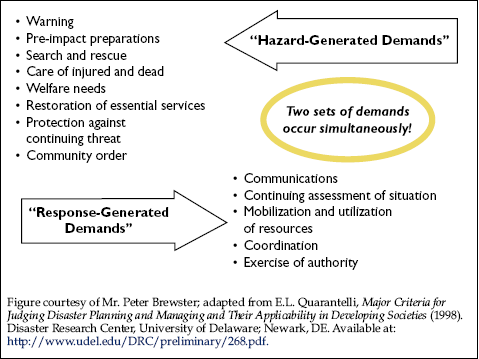
When an incident generates demands on the response system, the issues addressed first are usually demands created by the hazard itself—hazard-generated demands. For example, in a highly contagious disease outbreak, hazard-generated demands include the need to evaluate and treat victims, while controlling the spread of the disease. Simultaneously, the response system itself creates response-generated demands. In the same example, these demands include the need to coordinate disparate resources, to process widely dispersed data into accurate epidemiological information, to coordinate the public message, and to protect healthcare workers. Too often, the response community focuses on the hazard demands and neglects response demands until the latter create a significant impediment to overall response effectiveness. With well-developed ICS and emergency management support, the incident response proactively addresses both types of demands and, in fact, reduces many response-generated demands to routine status.
1.4 The Incident Command Process
The incident command process describes an ordered sequence of actions that accomplishes the following:
- Activates the system and defines the incident response structure
- Establishes incident goals (where the system wants to be at the end of response; these are referred to as "control objectives"[23] in NIMS) to any single operational period (thus distiguishing them from operational period objectives).
- Defines incident operational period objectives (measurable steps that contribute to reaching the goal) and strategies to meet the defined objectives
- Adequately disseminates information, including the following, to achieve coordination throughout ICS:
- Response goals, objectives, and strategies
- Situation status reports
- Resource status updates
-
Safety issues for responders
-
Communication methods for responders
-
Assignments with individual assignment objectives and operating parameters
- Evaluates strategies and tactics for effectiveness in achieving objectives and monitors ongoing circumstances
- Revises the objectives, strategies, and tactics as dictated by incident circumstances.
Actions during the initial phases of incident response should be guided by checklist procedures established in the EOP. For any response of more than a few hours, management should transition to a method of proactive response by establishing incident-wide objectives. These overarching "control objectives" are further qualified by establishing measurable and attainable objectives for each operational period, and by defined strategies and tactics. All are documented in an IAP. Because event parameters and the status of the components of an asset will change, incident objectives will have to change as the response evolves.
This flux in incident and response conditions is best managed using a deliberate planning process that is based on regular, cyclical reevaluation of the incident objectives. Commonly known in ICS as the planning cycle (see Figure 1-5), this iterative process enhances the integration of public health and medical assets with other response agencies that operate planning cycles.
Figure 1-5. Basic Presentation of a Planning Cycle.[24]
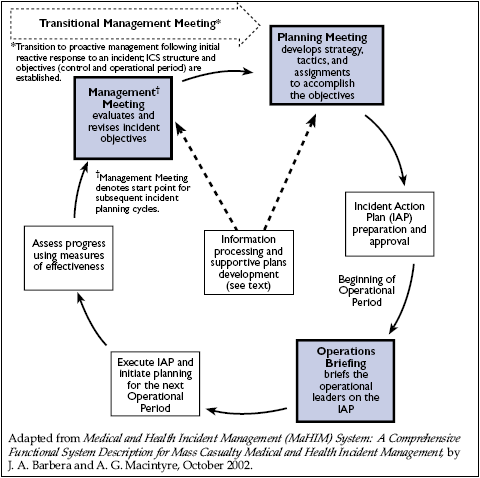
The timing of the development of incident action plans should be coordinated among disciplines so that updated information may be shared before strategies and objectives are established. As shown in Figure 1-5, the key steps in the planning cycle are:
- Transitional management meeting: This marks the transition from reactive to proactive incident management. The transitional meeting brings together the leadership of key response disciplines, defines the primary incident management team, and allows managers to be briefed on the known incident parameters. If the lead incident commander determines that formal incident planning is warranted, the command staff set initial incident goals (i.e., control objectives) and operational period objectives and the planning cycle process moves forward.
- Planning meeting: Using the objectives set during the transitional (or a subsequent) management meeting, the incident management team, with leaders of key functional areas, sets strategies, general tactics, and major assignments. These are documented by the Planning Section and become a central component of the IAP. For public health and medical disciplines, documentation of an IAP has rarely been undertaken as an essential action during response, and yet it is one of the most effective means for coordinating between multiple locations, resources, and levels of government (see
appendix C for an example of an IAP). The addition of supportive plans[25] completes the IAP for the upcoming operational period.
- Operational briefing: All components of the response system are briefed on the operational period objectives, strategies, tactics, and assignments. The purpose of the operational briefing is to impart information and to raise emergent issues, not to discuss alternative plans, debate choices made in the planning process, or undertake extensive problem solving. In traditional descriptions of ICS, the operational briefing occurs in person, but it may also occur telephonically or through electronic communications. A defined briefing process imposes discipline for the operational briefings so that time constraints are met, distractions are limited, and questions are kept to a minimum.
- Management meeting: This marks the onset of the next planning cycle. The incident command staff reevaluates the control objectives and progress made in meeting the operational period objectives, based on information collected throughout the operational period. Objectives are revised and new ones are established as appropriate.
The following critical points should be made about the planning cycle:
- Tiers, and assets within tiers, should attempt to coordinate their planning cycles with that of the primary incident command. This allows information exchange between assets and tiers to promote consistency in the development of incident objectives and strategies.
- A planning cycle is timed so the operational briefing occurs just before the beginning of work that is guided by the recently completed IAP. This work interval is usually referred to as an operational period. It is beneficial, therefore, for assets directly managed by the IAP to establish common operational periods.
- Throughout the action planning process, the Planning Section plays a critical role by stewarding the planning activities and processing data into information that is relevant to incident decision-making.
During an emergency, the normal administrative structure for an organization must continue to operate while actions are carried out under the EOP to address the incident. Issues not related to the incident are best managed, to the extent possible, by the usual, day-to-day administrative system. In a sense, the ICS structure works within and for the organization's usual administrative system. This concept may be obvious to some disciplines such as Fire Fighting (the entire Fire Department is not replaced by the ICS structure during response) but may not be as intuitive in the example of smaller organizations such as some healthcare facilities.
For this reason, it is generally NOT advisable for the Chief Executive Officer (CEO) or other senior executive to automatically assume the position of the Incident Commander (IC) for an organization. Instead, this individual may be better situated to serve in the role ICS denotes as "Agency Executive."[26]. This individual maintains overall authority and responsibility for the organization, including the activated incident management team. The executive is involved in the incident by providing policy and strategic direction to the IC, as well as allocating the authority to the IC to manage the incident. The Agency Executive must have access to the IC and may be included in the incident planning meetings.
This concept of an Agency Executive is important for organizations to understand as they seek to develop an effective EOP and interface with other organizations. Even though the ICS for the organization may be clearly delineated, the role of the Agency Executive is not always well addressed.
Multiple organizations may have leadership responsibilities during a mass casualty and/or mass effect event. ICS has a designated model, Unified Command (UC), which allows multiple stakeholders to actively participate in incident management. When this occurs, the resulting UC team promotes cohesive action within the response system, and provides a uniform interface for integration with other tiers. This concept is critically relevant for participation by public health and medical disciplines since they bear a primary responsibility for the well-being of responders and the general population during emergencies or disasters. The UC model provides a mechanism for direct input from public health and medical practitioners at the decision-making level.
UC brings together incident managers of all major organizations involved in the incident to coordinate an effective response, while allowing each manager to carry out his/her own jurisdictional or discipline responsibilities. UC links response organizations at the leadership level, thus providing a forum for these entities to make joint decisions. Under UC, various jurisdictions and/or agencies and non-government responders may work together throughout the incident to create and maintain an integrated response system. UC may be established to overcome divisions from:
- Geographic boundaries
- Government levels
- Functional and/or statutory responsibilities
- Some combination of the above.
(Adapted from: U.S. Coast Guard Incident Management Handbook, U.S. Coast Guard COMDTPUB P3120.17, April 2001)
Unified, proactive incident command is accomplished through joint decision-making that establishes common incident objectives (i.e., management by objectives). During an incident, clearly delineated goals and objectives are agreed on and formally documented to form the basis of the IAP. To accomplish this strategic guidance throughout an incident, UC must entail:
- A single integrated management structure for the emergency response
- Shared or co-located management facilities
- A single planning process and IAP (single set of goals and objectives)
- A coordinated process for requesting and managing resources.
As previously described, Command and Operations are primarily supported by three internal (within ICS) Sections: Logistics, Planning, and Administration/Finance. However, in large-scale or complex events, incident command may require additional support from entities outside the responsibility/authority of ICS. This commonly occurs through an emergency management operations function—known in NIMS as a Multiagency Coordination System (MACS)—that is usually based in an Emergency Operations Center (EOC).[27]. For Tier 3, it is usually supervised by the jurisdiction's emergency manager.
Figure 1-6. Relationship of UC and the MACS that provide emergency management operations support to the UC.
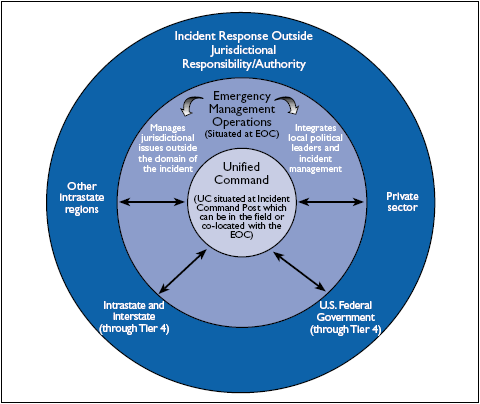
Multiagency Coordination Systems provide the architecture to support coordination for incident prioritization, critical resource allocation, communications systems integration, and information coordination.[28] The coordination center (EOC and others, see figure 1-7) is referred to in NIMS as the Multiagency Coordination Center (MACC) component of the MACS. It provides support and coordination to the Incident Command, facilitates logistical support, and develops and provides information. The component of the MACS that provides strategic decision-making and policy direction (senior policy groups and others) is referred to as the Multiagency Coordination Group (MAC Group).[29] The MACC implements the MAC Group decisions.[30]
Figure 1-7. Common types of Multiagency Coordination Groups and Centers[31]

During response, the MACS:
- Directly supports the UC by providing resources that are not available through incident-specific ICS capabilities. This includes coordinating assistance from outside resources (Federal, State, and other jurisdictions) that cannot be obtained through tactical mutual aid.
- Directly manages emergency issues related to the incident, but that are outside the scope of the incident as defined by the UC. This may be determined geographically (outside a scene perimeter) or functionally (beyond the scope of the UC control objectives when no single scene exists or when the impact is diffuse). An example is provided below.
- Provides integration between community political leaders and the incident managers.
Example: In the event of a widespread outbreak of SARS in a jurisdiction, the UC (with lead participation by public health and the acute-care medical community) would establish protocols to guide the medical evaluation and treatment of confirmed and suspected cases, and to address surge capacity needs. In addition, the UC would be responsible for limiting the spread of the disease (as defined by their IAP).
Addressing the needs of travelers stranded when mass transit is disrupted, addressing requests to minimize the effect of school or business closures, and other significant issues may be considered to be functionally outside the scope of the incident response system. The jurisdiction's EOC would manage these issues using its emergency management team and Emergency Support Functions (ESFs), or other task groups.
Because of its complex role, the EOC's organization and management processes must be well defined. The MACS functions should be physically separate from incident management activities, even if they are co-located in the same facility. This critical concept, which is not widely addressed by many medical and public health managers, ensures that the roles and responsibilities of each remain distinct.
1.5 Concept of Operations
The management process delineated in the MSCC Management System is best presented in relation to the various stages of incident response.
Figure 1-8. Stages of Incident Response
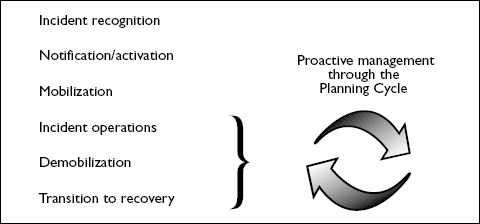
These stages provide the context in which to describe the critical actions that must occur at different times during incident response.
Incident recognition is the point in time when a response agency becomes aware that a significant event (i.e., one requiring emergency response beyond baseline operational capability) is imminent or occurring. This is not always obvious, particularly with the onset of an infectious agent or chemical toxin. For example, one or two patients presenting to scattered HCOs with progressive paralysis indicating botulism may not be immediately recognized as a major public health problem until they are linked to a single toxin source. Because of this potential ambiguity, the process used to move from an early suspicion to recognizing that incident response is indicated should be carefully considered. Early convening of the jurisdiction's (Tier 3) UC, for example, may provide the necessary understanding of any public health impact associated with an event, and it may clarify whether an event needs to be formally declared an emergency.
Notification/activation refers to the activities required to inform appropriate assets within the response system about an incident onset or an important change in incident parameters. "Notification" conveys critical details (if available) and an indication as to whether the notified asset should undertake response actions. Full activation of every response component under UC is often not necessary and, therefore, the activation request in each asset's notification message may vary depending on the type of event.
Many notification/activation categories and schemes have been promulgated. Those selected for use should be consistent within tiers and easily understood across other tiers. To further prevent confusion, the categories should be clearly defined on each communication. The Federal Urban Search and Rescue System (and other Federal agencies) have used one notification/activation categorization for over a decade because of its clarity and simplicity.
Federal Urban Search and Rescue Notification/Activation Categories:
- Advisory: Provides urgent information about an unusual occurrence or threat of occurrence, but no significant action is recommended, requested, or required.
- Alert: Provides notification of an unusual occurrence where a response is anticipated or indicated. It provides guidance on the degree of action to take at the time of the alert. In some systems, an alert from a designated agency also authorizes the expenditure of a specific funding amount to address the costs of the requested pre-mobilization actions.
- Activation: May be either partial or full:
- Partial: Specific components or assets within a unit are activated (all other components should receive notification regardless of their activation status).
- Full: All resources commence response according to procedures described in the asset's EOP.
Other information is conveyed through "updates" during the course of the incident response.
Sources: Adapted from FEMA Urban Search and Rescue System; J. A. Barbera and A. G. Macintyre. Jane's Mass Casualty Handbook: Hospital; Jane's Information Group, Ltd., Surrey, UK, 2003.
The notification process should include a "confirmation of receipt" reply from the intended recipient. This reply should also contain a brief status report from the notified asset (using a standard format developed during preparedness planning) to allow immediate assessment of the response asset's capabilities.
Mobilization marks the transition from baseline operations to the response level designated in the notification. It may be triggered by a hazard that has already occurred, or it may result from a credible threat or an impending hazard (such as an approaching hurricane). Designating the response level enables an organization to execute specific actions delineated in its EOP for that level, such as providing contact information to ensure that the asset can integrate with other mobilizing response entities. For the mobilization process to function efficiently, each step must be clearly defined during preparedness planning and staff must learn the steps through training.
Incident operations encompasses efforts that directly address the hazard impact. Two critical actions that should occur early during operations are:
- Establishment of incident management authority: For certain types of incidents, the lead management authority and how incident management will be conducted are relatively straightforward (e.g., local fire service usually manages an explosion at a shopping mall). Management authority is more ambiguous in events that extend across jurisdictional boundaries or authorities (e.g., bombing at a Federal facility) or when the impact is diffuse (e.g., disease outbreak in multiple State jurisdictions). For most major incidents, tradition (and successful previous experience) dictates that jurisdictional authorities are responsible for incident management. For a diffuse impact scenario, State public health authorities (in a UC model similar to "area command" described in NIMS) might assume the lead role in UC and coordinate the incident response across the affected jurisdictions.
- Establishment of Incident Command Post: The site where the primary incident management team will function must be rapidly established and publicized across the response system. During any sudden onset or large-scale incident, several initial management sites are often established and operated by multiple disciplines from a range of MSCC tiers. The terminology used to designate them may not reflect their actual roles. Thus, identifying and publicizing the primary management site and how it integrates the other sites is a critical task in organizing incident-wide, proactive management.
When incident response involves multiple disciplines and levels of government, it becomes operationally important to synchronize, as much as possible, the planning activities of participants so that response actions can be coordinated (Figure 1-9). This promotes consistency across tiers in defining the incident objectives and follow-on tactics. It also ensures consistency in the development of public messages.
As Figure 1-9 shows, the planning cycles and operational periods for the jurisdiction (Tier 3) and State (Tier 4) are concurrent; those for the Federal response (Tier 6) are slightly staggered. This allows for information exchange during planning activities. The agency representative meeting enables the evolving IAP to be reviewed in time to identify conflicts before briefing the operational units. This meeting can be conducted face-to-face or via teleconference. A formal media briefing to release incident details could occur after the agency representative meeting to ensure that responders are informed first and to promote a consistent message.
Figure 1-9. Coordination of Planning Activities
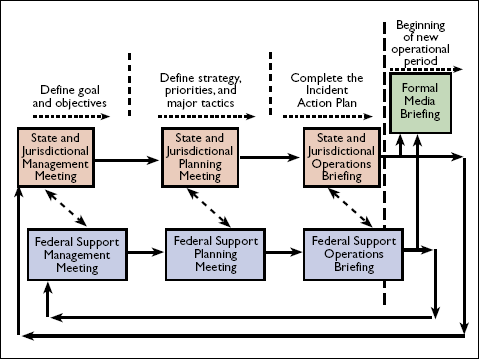
Demobilization refers to activities that focus on disengaging response resources as the incident objectives are met, transitioning remaining incident responsibilities to ongoing assets, and promoting rapid return of demobilized response resources to their normal function. There are several important considerations:
- Demobilization across assets: The timing of resource demobilization is a complex and difficult decision, with potentially competing priorities between incident managers and managers of individual assets. The managers of individual assets and agencies should always coordinate any decision with the overall incident command. Demobilization of individual assets may occur at widely varying times, with some taking place early in a response if objectives have been met.
- Representing demobilization to the media and public: Management of the public's perception of asset demobilization may be very important, depending on the incident and the asset (e.g., the public believing the event is not over, thus being dismayed that an asset is disengaging). This should be considered carefully and addressed through incident management processes, including public information action that demonstrates that the asset's objectives have been accomplished and it is no longer needed.
- Continued use of ICS during demobilization: For medical resources, demobilization (and initial recovery) must occur efficiently because medical backlogs created during response can present a significant risk to the asset's regular patient population (e.g., delays in performing cardiac catheterizations), as well as a financial risk (e.g., loss of revenue from elective surgery). The continued use of ICS processes may be beneficial in addressing backlogs and should be considered during planning for both individual asset and overall incident demobilization.
Recovery refers to longer-term activities that extend beyond demobilization and other response activities. It includes the rehabilitation of personnel and equipment, resupply, and actions related to physical and financial restoration. Returning the overall system to its pre-incident state—the goal of the recovery stage—is addressed by developing and implementing strategic plans for full restoration and system improvement.
Post-incident "organizational learning" is achieved through a timely and objective after-action report process that is designed to capture the positive aspects and the shortcomings of the response system. Findings should be documented in an outline format that can be organized on a spreadsheet and tracked. One basic format that has been widely successful is designed to capture, for each issue, a brief description of the issue, background information, recommendations, and follow-up actions. Improvements should focus on the EOP organization, processes, and training or equipment/supply issues, rather than on individual personnel actions. The review should also examine how effectively each asset integrated into the overall system, as well as how the response tiers coordinated with each other. Indicated changes should be accomplished based on priority and incorporated into the appropriate documentation.
1.6 The Public-Private Divide
This chapter has presented several key concepts of ICS on which the MSCC Management System is based. A difficulty with applying traditional ICS in major medical and public health incidents is that it is designed primarily for management participation by public safety personnel. It is difficult within ICS to identify defined mechanisms for incorporating private sector assets into incident management, even if they are essential in providing leadership-level expertise for the incident. This problem was apparent in New York City after 9/11, where it was challenging to efficiently incorporate engineering deconstruction expertise (largely a private sector asset) into incident management.[32] This issue is particularly problematic for medical input into incident management because specialty medical expertise in the United States resides primarily in the private sector.
The World Trade Center experience in the aftermath of 9/11 and the response to Hurricane Katrina demonstrated many factors that can exacerbate the public-private divide:
- Private assets may have conflict-of-interest issues when participating in public management.
- Public agency officials may be reluctant to accept high-level management advice because they may not be comfortable with the source's objectivity or expertise. This is more likely if in-depth familiarity was not established during preparedness planning.
- Private-sector assets do not have the liability immunity for public management that is enjoyed by public officials when acting within their established capacity. This may create a reluctance to engage in public decision-making without reliable assurance that they will not incur unacceptable legal risk.
Response systems for public health and medical incidents must identify and implement methods to bridge the public-private divide. Depending on the type of incident, qualified medical experts may provide strategic advice through a formal position in UC or as senior advisors to the UC. Alternatively, they may serve as technical specialists when their input is provided at a tactical level. Regardless of the approach, qualified medical experts must know when and how to interface with incident management (as they are rarely in charge of major response), and understand other implications of mass casualty and/or mass effect events. These experts should be selected from the medical community for their ability to accurately and fairly represent the collective interests of the private sector by providing the following:
- Advice as it relates to medical operations
- Evaluation of management options for addressing medical issues
- Peer review of public messages for medical accuracy and clarity
- Peer review of messages to the professional medical community to promote accuracy of the message and acceptance by participating medical responders
- Other assistance or expertise, as indicated.
12. A mass effect incident may be defined as a hazard impact that primarily affects the ability of the organization to continue its usual operations (in contrast to a mass casualty incident). For healthcare systems, the usual medical care capability and capacity can be compromised and the ability to surge prevented.
13. Throughout this document, the term adequate implies a system, process, procedure, or quantity that will achieve a defined response objective.
14. Readers are encouraged to visit the
Agency for Health Research and Quality Web site (http://www.ahrq.gov/) for information on alternate care facilities and allocation of scarce resources.
15. Traditionally, patient needs are matched with available resources by evenly distributing large numbers, or very ill/injured patients, to available facilities. This is logistically difficult because, in a mass casualty and/or mass effect incident, many victims self-refer for medical care (i.e., arrive outside the formal EMS system).
16. Cooperative agreements provide the same services as mutual aid, but they establish a mechanism for payment for the responding services by the affected jurisdiction. This may also be referred to as "reimbursed" or "compensated" mutual aid (the term "mutual aid" otherwise implies assistance without remuneration).
17. The authority for the Secretary of HHS to declare a Federal public health emergency or disaster is granted under Section 319 of the U.S. Public Health Service Act.
18.Appendix A highlights several critical assumptions that were made in developing the MSCC Management System.
19.Appendix B describes the basic ICS for public health and medical personnel.
20. Many of these procedures increase the efficiency of preparedness activities, while essentially training participants on the procedures to be used during response and recovery. Examples include the use of emergency notification procedures for disseminating preparedness information, the use of a management- by- objective approach when planning preparedness tasks, and using tightly managed meetings with detailed agendas.
21. A function is a key set of tasks that must be performed during incident response. They are grouped according to similarity of purpose but are not positions, per se, because each could entail multiple persons working to fulfill that function.
22. Key components of an incident action plan are presented in
Appendix C.
23. "Control objectives" is the NIMS term for overall incident response goals and are not limited
24. While ICS descriptions of the meetings in the planning process vary across versions, this diagram encompasses the principle actions in all versions of the ICS planning cycle.
25. Supportive plans include the Safety Plan, the Medical Plan (for responders), communications plan, contingency plans, and others.
26. Agency Executive is defined as the Chief Executive Officer (or designee) of the agency or jurisdiction that has responsibility for the incident (FEMA ICS definition).
27. Additional information on MACS can be found in Chapter 2 of the NIMS
28. The components of MACS (per NIMS) include facilities, equipment, emergency operation centers (EOCs), specific multiagency coordination entities, personnel, procedures, and communications. These systems assist agencies and organizations to fully integrate the subsystems of the NIMS (NIMS glossary).
29. Multiagency Coordination Group: A Multiagency Coordination Group functions within a broader multiagency coordination system. It may establish the priorities among incidents.
30. ICS 300 Unit 5: Multiagency Coordination; available through FEMA Emergency Management Institute, Emmitsburg, MD.
31. ICS 300 Unit 5: Multiagency Coordination; available through FEMA Emergency Management Institute, Emmitsburg, MD.
32.This observation was made by Dr. Joseph Barbera, who was present at the World Trade Center site in the days and weeks following the attacks.

